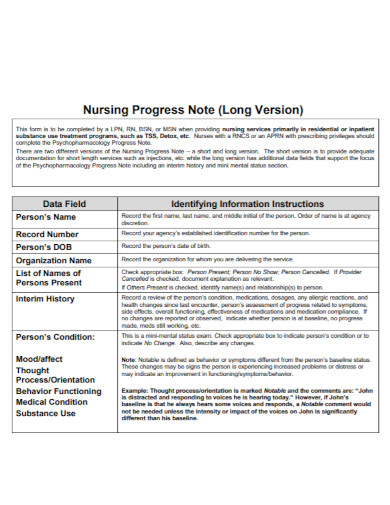
The transition from caregiving to independent living presents a significant shift for individuals with dementia and other cognitive impairments. Effective communication and documentation are paramount during this period, and a well-structured ‘Progress Notes Aged Care Template’ is an invaluable tool for healthcare professionals, caregivers, and families. This template provides a standardized framework for recording vital information, facilitating continuity of care, and supporting informed decision-making. It’s more than just a record; it’s a lifeline, ensuring that the individual’s needs are understood, addressed, and continually monitored. The core purpose of this template is to streamline the process of capturing essential details, promoting clarity, and maintaining a comprehensive understanding of the individual’s condition. Progress Notes Aged Care Template – a simple yet powerful tool for preserving valuable insights.
The initial implementation of a standardized template is crucial for several reasons. Firstly, it reduces the risk of fragmented information, which can lead to miscommunication and potentially detrimental errors. Secondly, it allows for a more consistent and objective record-keeping process, minimizing subjective interpretations. Thirdly, it facilitates collaboration among different caregivers, healthcare providers, and family members, ensuring everyone is on the same page regarding the individual’s status and needs. Furthermore, utilizing a template encourages a systematic approach to documentation, promoting a more organized and efficient workflow. The benefits extend beyond simple record-keeping; it fosters a sense of security and predictability for both the individual and their loved ones. A clear and documented record provides a foundation for proactive care planning and adjustments.

A comprehensive ‘Progress Notes Aged Care Template’ typically includes several key sections. Each section is designed to capture specific aspects of the individual’s daily life, activities, and any observed changes. The specific content required within each section will vary depending on the individual’s needs and the care plan in place. However, some core components are consistently essential. The first section, often called the “Presenting Problem,” details the current situation, including any recent changes in behavior, cognitive function, or physical condition. This section is vital for identifying potential triggers and understanding the underlying causes of any concerns. Next, the “Assessment” section provides a detailed evaluation of the individual’s current state, incorporating observations, relevant data, and any relevant information gathered from caregivers, family members, or healthcare professionals. This section is a critical opportunity to document the individual’s strengths, weaknesses, and any areas requiring attention. Finally, the “Plan” section outlines specific actions, goals, and strategies to address the identified needs and maintain the individual’s well-being.
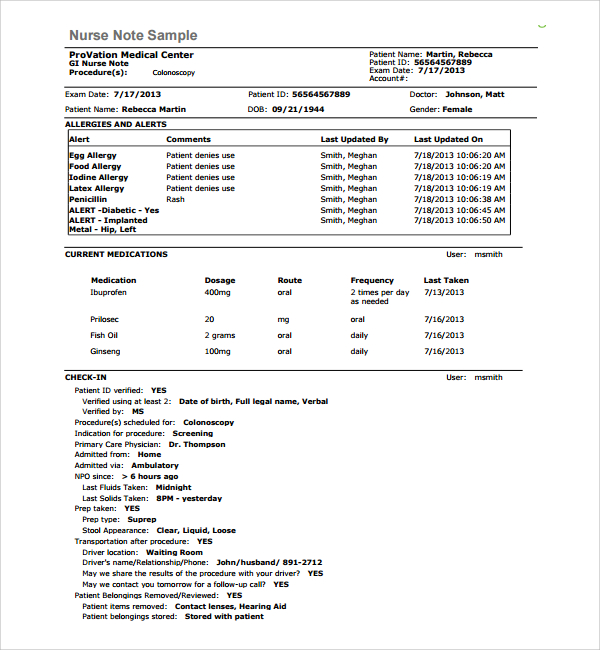
This section is the cornerstone of the ‘Progress Notes Aged Care Template’ and requires meticulous attention. It’s not simply a list of symptoms; it’s a holistic representation of the individual’s current situation. It should include:

The assessment section is where the ‘Progress Notes Aged Care Template’ goes beyond simply describing observations; it provides a structured evaluation of the individual’s condition. It should include:

The ‘Progress Notes Aged Care Template’ culminates in a clear and actionable plan, outlining specific steps to address the identified needs and maintain the individual’s well-being. This section should include:

Beyond the core sections, consider incorporating these additional elements:
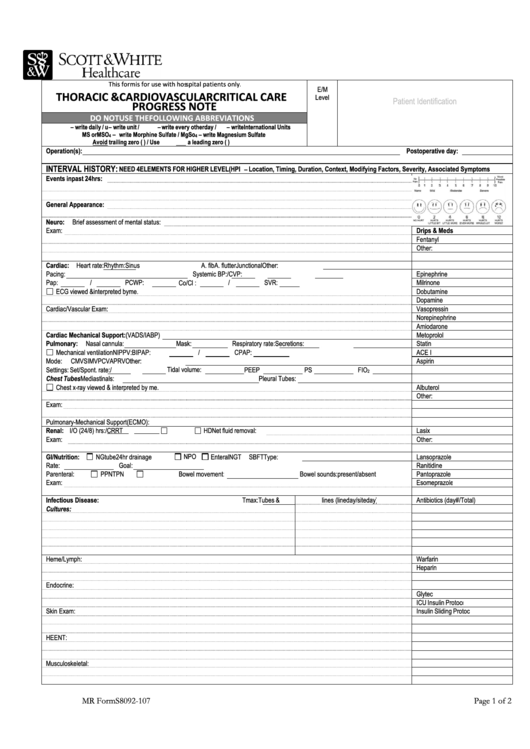

The ‘Progress Notes Aged Care Template’ is a dynamic and evolving tool, designed to support individuals with dementia and other cognitive impairments throughout their lives. It’s a crucial component of comprehensive care planning and a vital resource for caregivers and healthcare professionals. By consistently utilizing this template and adapting it to the individual’s unique needs, we can promote optimal care, enhance quality of life, and ensure a more fulfilling experience for everyone involved. Ultimately, the goal is to provide a clear, objective, and compassionate record of the individual’s journey, fostering a deeper understanding of their condition and facilitating proactive and responsive care. The consistent application of this template, coupled with ongoing communication and collaboration, is essential for achieving positive outcomes. The continued refinement and adaptation of this template will undoubtedly contribute to improved care delivery and enhanced outcomes for individuals navigating the complexities of aging.