In high-stakes environments where a single miscommunication can have significant consequences, structured communication is not just a best practice—it’s a necessity. For healthcare professionals, ensuring that critical patient information is conveyed clearly, concisely, and completely is paramount to patient safety. This is where a customizable Sbar Template Word document becomes an indispensable tool, transforming a proven communication framework into an accessible and practical daily resource. By leveraging a simple yet powerful template, clinical teams can standardize handoffs, streamline calls to physicians, and ultimately reduce the risk of medical errors.
The SBAR framework—an acronym for Situation, Background, Assessment, and Recommendation—is a standardized communication model developed by the U.S. Navy for use on nuclear submarines and later adopted by the healthcare industry to improve patient outcomes. Its genius lies in its simplicity and logical flow, creating a shared mental model that helps all parties quickly grasp the most important information. While the SBAR method can be used verbally from memory, institutionalizing its use through a standardized template ensures that no critical element is forgotten, especially during stressful or time-sensitive events.

This guide will provide a comprehensive overview of the SBAR framework and explore the immense value of using a Microsoft Word template to implement it. We will walk through the essential components of SBAR, detail the benefits of a digital template over paper-based or ad-hoc methods, and provide a step-by-step guide to creating and customizing your own template. Whether you are a nurse manager looking to improve unit-wide communication, a resident physician aiming for more efficient handoffs, or a healthcare administrator focused on quality improvement, this article will equip you with the knowledge to effectively deploy SBAR in your clinical practice.

Before diving into creating a template, it’s crucial to have a solid understanding of the SBAR framework itself. SBAR provides a structured format for organizing and conveying information, which helps eliminate vague language and ensures the recipient understands the urgency and context of the situation. Endorsed by leading healthcare organizations like The Joint Commission and the Institute for Healthcare Improvement (IHI), its effectiveness is rooted in its four distinct components.

This is a concise, one-sentence statement that immediately identifies who you are, where you are, who the patient is, and what the core problem is. The goal is to grab the listener’s attention and frame the conversation. It should be direct and to the point.

This section provides the essential context and relevant history needed to understand the situation. It should be brief but comprehensive, including information that is pertinent to the current problem. Avoid extraneous details that could cloud the main issue.

Here, you present your professional clinical assessment of the situation. This includes the most recent vital signs, lab results, and your interpretation of what is happening. This is where you connect the dots between the background information and the current situation.
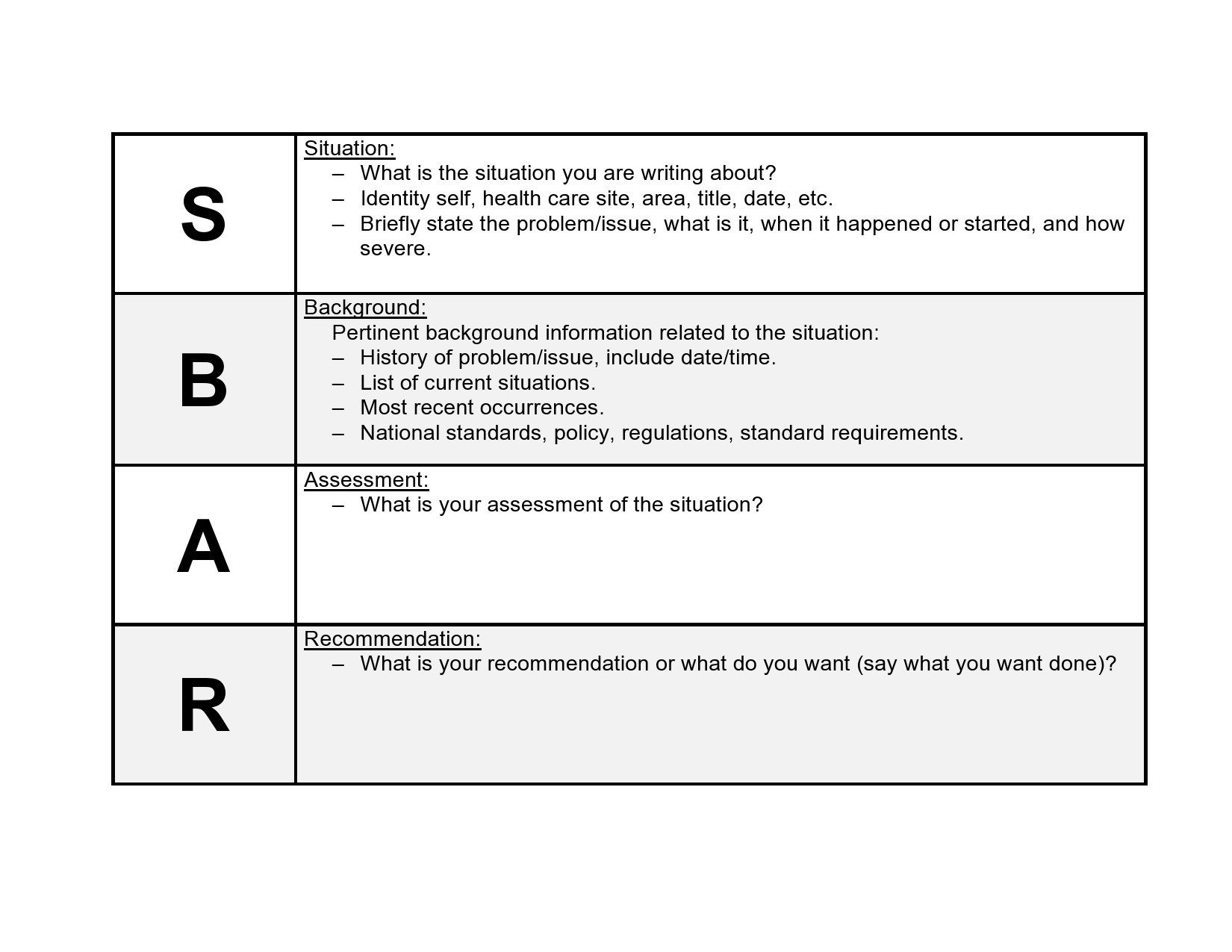
Finally, you clearly state what you need from the other person. This is your call to action. Be specific and direct in what you are requesting, whether it’s a new order, a specific action, or for the provider to come and see the patient.

While verbal SBAR is effective, a digital template elevates its utility to a new level. Using Microsoft Word to create a standardized form offers numerous advantages that enhance consistency, efficiency, and patient safety across a team or an entire facility.

Human memory is fallible, especially under pressure. A template acts as a cognitive aid and a checklist, ensuring that no critical piece of information—from allergies and code status to key lab values—is omitted. Every handoff and every call follows the same predictable, high-quality format, reducing variability and the risk of miscommunication.

A well-designed template allows clinicians to gather and organize their thoughts before initiating communication. Instead of scrambling for information during a call, a nurse can pre-populate the template with the patient’s vitals, lab results, and medication times. This preparation leads to more focused, concise, and professional conversations that respect everyone’s time.
Unlike generic paper forms, a Sbar Template Word document can be easily modified to fit the unique needs of different departments or clinical situations. An ICU handoff template might include fields for ventilator settings and drips, while a long-term care template might focus more on changes in functional status. This flexibility ensures the tool remains relevant and practical for its intended users.
Illegible handwriting on handoff sheets is a notorious source of medical errors. A typed template eliminates this problem entirely. Furthermore, the completed digital document can be printed and placed in the patient’s chart (per facility policy) or saved electronically, creating a clear and permanent record of the communication that took place.
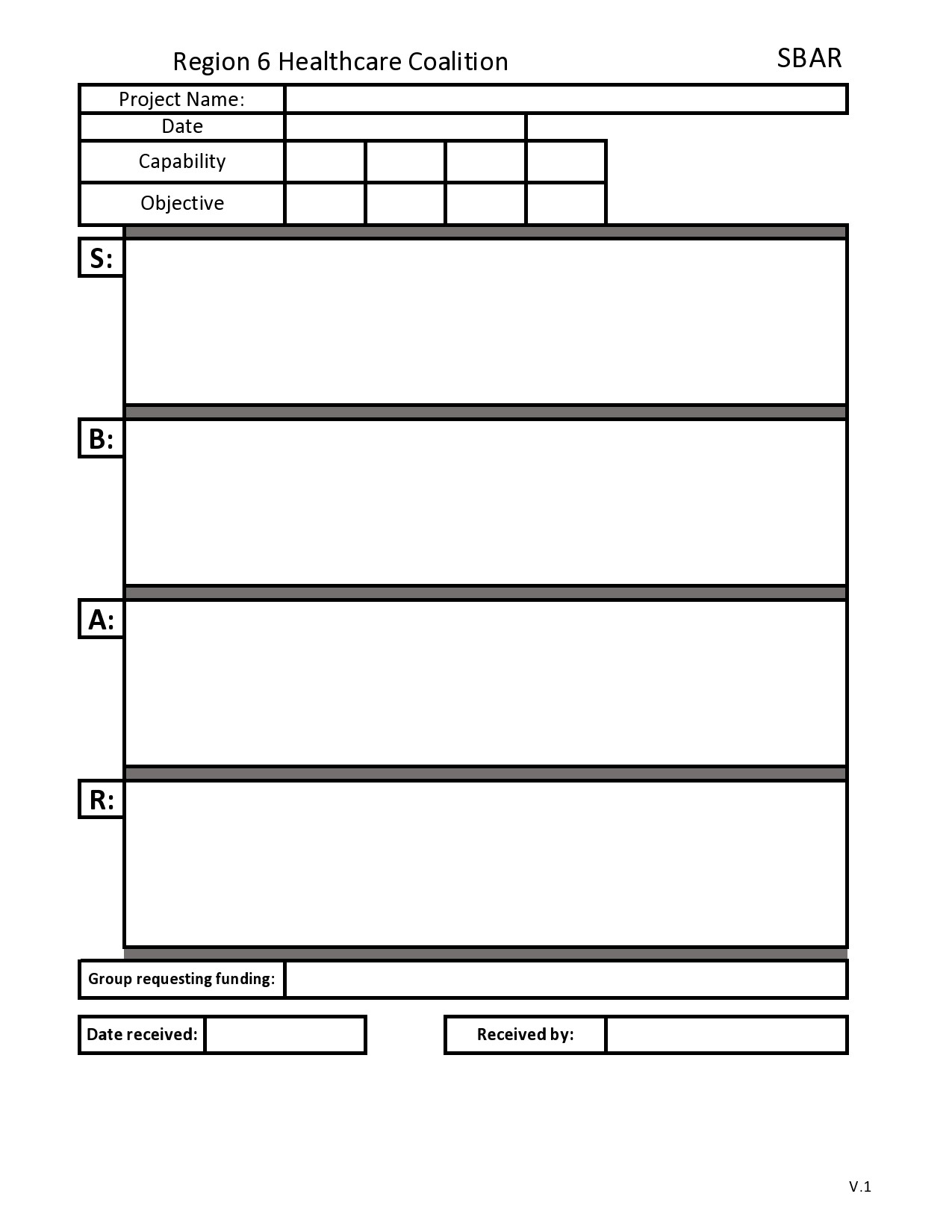
Creating a functional and user-friendly SBAR template in Microsoft Word is a straightforward process. The key is to balance structure with enough flexibility for clinical judgment. A table-based format is often the cleanest and easiest to use.
Start by opening a new blank document in Word. The first thing you should create is a header section for essential patient identifiers. This ensures the most critical information is visible at a glance.
Include fields for:
* Patient Name:
* Date of Birth (DOB):
* Medical Record Number (MRN):
* Room Number:
* Admitting Physician:
* Code Status: (e.g., Full Code, DNR)
* Allergies:
Insert a table with two columns and four rows. The left column will label the SBAR component, and the right column will provide space for the user to type.
In the right-hand column for each section, you will add prompts to guide the user.
This is the most important step. Add bullet points or checklist-style prompts within each cell to ensure all relevant information is captured.
For the Situation Cell:
* My name is: ____________ and my role is: ____________
* I am calling about patient: ____________ in room: _____
* The primary problem I am calling about is: ________________________
For the Background Cell:
* Date of Admission: __________ Admitting Diagnosis: ________________
* Relevant Past Medical History: ____________________________________
* Brief Summary of Hospital Course: ________________________________
* Relevant Medications/Treatments: ________________________________
* Most Recent Key Lab/Diagnostic Results: _______________________
For the Assessment Cell:
* Current Vital Signs: BP: __/__ HR: ___ RR: ___ Temp: ___ O2 Sat: ___ on __________
* Pain Level: ___ /10
* Physical Exam Findings: (e.g., Neurological, Respiratory, Cardiac) ________________
* My clinical assessment is that the problem is: __________________________
* The patient’s condition seems to be: (e.g., Stable, Worsening, Unclear) ___________
For the Recommendation Cell:
* I am requesting that you: (e.g., come see the patient, provide new orders) __________
* Are there any tests/labs you would like to order? ____________________
* What is the desired time frame for this action? _________________
* Read-back confirmation of orders received: ______________________
This is a critical final step. Do not save the file as a standard Word document (.docx). Instead, go to File > Save As and change the “Save as type” dropdown to Word Template (.dotx). When you save it as a template, every time someone double-clicks the file, it will open as a new, untitled copy. This preserves your original blank template from being accidentally overwritten.
Creating the template is only half the battle. Successful implementation requires clear guidelines and consistent practice to embed SBAR into your team’s workflow and culture.
Don’t just email the template to your team. Hold a short in-service or meeting to explain the purpose of the template and walk through each section. Use role-playing exercises with realistic clinical scenarios to help staff become comfortable with the format.
The primary benefit of the template is preparation. Encourage staff to take a few minutes to gather all the necessary data and fill out the SBAR form before picking up the phone or approaching a colleague for a handoff. This leads to a more organized and effective transfer of information.
The “Recommendation” section is perfect for practicing closed-loop communication. When receiving verbal or telephone orders, the clinician should write them down in the template and then read them back to the provider to confirm accuracy. This simple step is a powerful safety measure that prevents medication errors and other misunderstandings.
A template should be a living document. After the template has been in use for a few weeks or months, solicit feedback from your team. Are there fields that are consistently left blank? Is there critical information that is missing? Periodically review and revise the template to ensure it continues to meet the needs of your clinical environment.
The true power of a Word template is its adaptability. A single, one-size-fits-all form may not be optimal for every type of communication. Consider creating specialized versions for common scenarios.
A template for bedside shift report might include more detailed sections for pending tasks, family concerns, and a 24-hour care plan summary. It could also have a checklist for safety items like verifying IV lines, checking wound dressings, and ensuring call bells are within reach.
When transferring a patient to a different level of care (e.g., from the floor to the ICU), the SBAR needs to be extremely detailed. The “Background” section should be expanded to include a comprehensive summary of the hospital stay, and the “Situation” must clearly articulate the reason for the transfer.
In an emergency, communication needs to be lightning-fast and highly focused. A rapid response SBAR template might be more condensed, using checkboxes and minimal free-text fields to convey the most critical information—the immediate problem, vital signs, and suspected cause—in under 30 seconds.
Effective communication is the bedrock of patient safety. The SBAR framework provides a simple yet robust structure for conveying critical information, and leveraging a Sbar Template Word document makes this powerful tool practical, consistent, and accessible for everyday clinical use. By standardizing the flow of information, these templates reduce ambiguity, minimize the risk of omitted details, and empower clinicians to communicate with confidence and clarity.
Creating a custom template is a simple technical task, but its impact on team collaboration and patient outcomes can be profound. It transforms an abstract communication theory into a tangible workflow tool that supports better decision-making, fosters a culture of safety, and ensures that every patient’s story is told accurately and completely, every single time. By investing the time to develop, implement, and refine an SBAR template, healthcare teams take a significant step toward excellence in clinical communication.